In April 2020, with the COVID-19 pandemic in full force, hospitals across the country were filled with patients, often to capacity, while healthcare staff were stretched thin and requests for their time and talents were being made from all sides.
With these challenges and constraints in mind, one GetWellNetwork Defense Health Agency (DHA) hospital client began looking for ways to increase mobility activities for patients with COVID-19 admitted to their facility.
The benefits + challenges of exercise therapy for COVID-19 patients
Research demonstrated that patients with COVID-19 admitted to the hospital — who were well enough to sit up in bed and/or sit at the side of the bed — would benefit from simple short periods of exercise therapy to maintain mobility and avoid muscular atrophy. The same study recommended active mobilization where it could be implemented, including a range of activities like:
- Bed mobility activities
- Active range-of-motion exercises
- Active (assisted) limb exercises
- Activities-of-daily-living training
- Transfer training
- Cycle ergometer
- Pre-gait exercises
- Ambulation
Increasing opportunities for movement for patients with COVID-19 during their hospital stay quickly became a crucial part of the patient recovery process.
However, hospital staff faced the challenge of an increasing need for care team interaction to assist with this task of increased patient exercising at a time where hospital staff was spread to capacity and volunteer assistance was not an option due to the impact of the COVID-19 pandemic.
In practice: scaling care teams with technology to provide exercise therapy
A hospital team of nurses and physical/occupational therapists sought assistance from GetWellNetwork to automate their mobility solution and digitally deliver it to patients in their rooms.
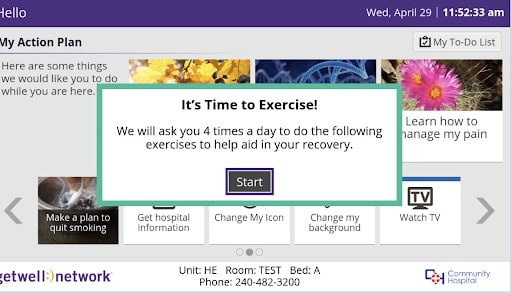
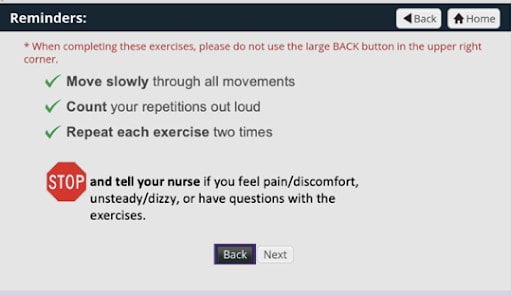
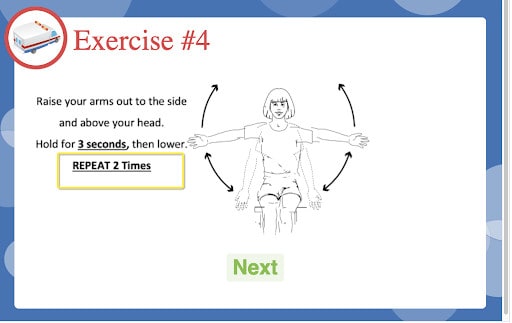
Using GetWell Inpatient, mobility instructions were delivered to patients on a specific sequence of exercises that could be performed individually without assistance.
Ensuring the best clinical fit
Clinically, it was clear that any kind of exercise therapy program could not be sent out to patients without a system in place to evaluate each patient and determine if digital prompting would be a good fit for their case.
Once a simple baseline level of acceptable bedside exercise activities was agreed upon by the facility care team, a workflow was implemented. Prior to a patient being identified as a candidate for the program, physical therapy, occupational therapy, and nursing would meet on a routine basis to discuss applicability for each patient’s needs.
When a patient was identified by hospital staff as able to safely navigate the independent exercise program from the bed, the GetWellNetwork bedside exercise program was activated. The patient received a series of five movements to help improve their overall physical well-being and ease them into more activity.
The bottom line
To date, there have been more than 2,050 patient interactions from this program at the DHA hospital. The program is an example of a best practice that can be digitally deployed when clinical and staffing needs require alternative methods for delivering physical and occupational therapy. And, in the time of a global pandemic, an all-hands-on-deck approach that includes digital healthcare technology can help scale care where it is needed most.
About the Author
Tina Grell, Client Success Manager, Government, has been working on behalf of GetWellNetwork’s government clients for nearly eight years. She is passionate about working with her clients to help them meet the unique challenges healthcare brings their way every day. A Veteran herself, Tina is also married to a Veteran and comes from a long line of military service members, including her father, brother, and grandfathers. She considers it an honor to be able to continue to serve by helping to bring the best technology that the healthcare industry has to offer into the government space.
