Improving the Veteran patient experience is a key aim for both the U.S. Department of Veterans Affairs (VA) and the team at Get Well. And part of shaping a better patient experience means offering top-notch, accessible patient education — digestible information that explains a patient’s condition, lets them know about symptoms to look out for, and informs them about different courses of treatment that may be offered. We know that an improved patient experience — and well educated patients — means that patients are more involved in their care and thus more likely to adhere to care plans, which leads to improved outcomes.
Patients who adhere to their care plans also see a reduction in harm. This is critical for the safety goals of the VA and its counterpart, the Veterans Health Administration (VHA). In February 2019, the VHA launched a High Reliability Organization (HRO) transformation initiative, committing to the long-term pursuit of a goal of Zero Harm. The VHA defines an HRO as “an organization that experiences fewer than anticipated accidents or events of harm despite operating in highly complex, high-risk environments where even small errors can lead to tragic results.”
In practice: Why tackle readmissions?
In response, one West Coast VA Medical Center partnered with Get Well to decrease heart failure readmissions for a national HRO readmissions collaborative. A multidisciplinary work group — including members of the VA team and representatives from Get Well — identified patient education as one area for intervention. Consistently automating Veteran patient education became a “proof of concept” project for system utilization for this VAMC. The goal was to help reduce heart failure readmissions by ensuring patients are educated during their stay on how to manage their diagnosis post-discharge so they do not end up back in the hospital.
Reducing readmissions for heart failure is a crucial quality improvement endeavor for many healthcare systems, including the VA. In combination with other interventions, patient education has been proven to help reduce readmissions. This approach aligns with the Get Well philosophy that an engaged and educated patient has better health and safety outcomes.
If the patient is educated during their hospital stay about their diagnosis (such as heart failure, in this instance), how to care for themselves, and how to identify signs their condition is worsening early on, then they are more likely to manage their health better post discharge. This care management minimizes progression of the disease process, and the patient can contact their primary care provider before they are so sick they need to be admitted again.
For the VA, publicly reported Strategic Analytics for Improvement and Learning (SAIL) reports are meant to represent the quality of care at each facility. Particular measures include hospital-wide 30-day readmission rates in addition to disease-specific 30-day readmission rates, including a report-out for congestive heart failure readmission rates (CHF RSRR).
By focusing on making patient education at its facility both high-quality and consistently assigned, this VAMC sought to lay the groundwork for lowered readmission rates for its Veteran population.
A lack of standardized education process led to low completion
Patients with heart failure who are admitted to the VA may receive education from their primary care team or from the nursing staff. Because there is no standardized process for providing this education, the quality and quantity of patient education are extremely varied.
There are systemic issues for this uneven implementation, as well, including:
- Clinical workload: Providers and other healthcare staff may have too many tasks on their metaphorical plates to cover during rounds to also add on patient education, whether at bedside or via digital assignment.
- Staffing issues: Particularly with the staffing shortages brought on by the COVID-19 pandemic and facility turnover, many institutions find themselves short-staffed, meaning remaining healthcare staff may be strapped for time and unable to take on extra patient education.
- Lack of standardized educational script: Without talking points for each type of patient education, staff are left to interpret materials as they see fit, leading to inconsistent application.
Creating a pathway to educate our Veterans
Although GetWell Inpatient, Get Well’s digital patient education platform, was implemented at this West Coast VAMC nearly 10 years ago, physicians nevertheless struggle to place the orders to launch patient education.
Recognizing a missed opportunity to provide patient education to Veterans through the hospital stay, the multidisciplinary HRO readmissions team aimed to improve heart failure education for Veterans by creating an automated and standardized education pathway through GetWell Inpatient.
Working together, the advanced heart failure team, the HRO team, and Get Well created a concise and complete educational pathway that includes educational videos. The videos included an explanation of a heart failure diagnosis, treatment modalities, and warning symptoms.
Human factors engineering principles, or human-centered design, played a large role in the implementation of the GetWell Inpatient education heart failure pathway. Human Factors principles seek to reduce human error, increase productivity, and enhance safety and comfort between a human and technology.
Using these principles, the team worked with the VAMC’s Information Technology division and Get Well to create an automated order for the pathway that would be triggered by a telemetry order with the indication of “Acute CHF.” This automation would remove the need for a provider to remember to proactively order the education.
Promising engagement results in a short span of time
In the six months preceding the initiation of the pathway, November 2021 – February 2022, there were 0 videos viewed by patients. Since the automated heart failure education pathway effort began at the end of March, there have been 53 individual videos watched, with the monthly number rising with each successive month.
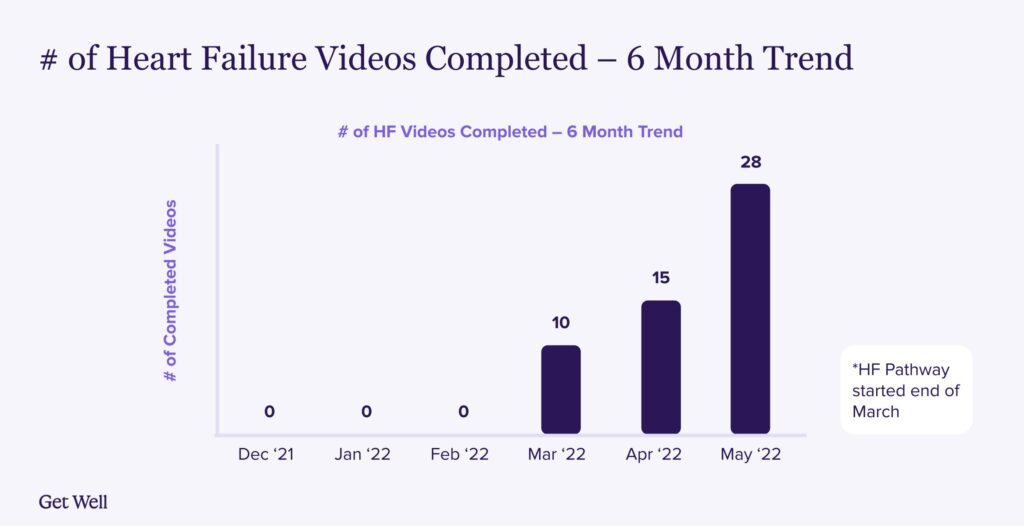
This effort is currently focusing on the number of videos viewed during the early stages of the project, but long-term data collection will focus on patient experience data and readmission data.
The bottom line
By increasing the opportunity for patient education in a standardized and automated fashion, this West Coast VAMC hopes to improve the overall patient experience and, ultimately, lower readmission rates for its Veteran population. The personalized, proactive, and patient-driven approach to surfacing education for all who need it is a good first step.
