Why GetWell Navigate
The healthcare landscape is more fragmented than ever, which means that the healthcare experience is also fragmented. People often struggle to know where to go, what resources to use, and who they can trust. Too often, patients don’t feel like they are treated as people.
But providing whole-person, personalized care is not only the right thing to do. It sets apart leading healthcare organizations. Get Well’s digital patient navigation solution, GetWell Navigate, helps organizations bridge gaps in critical areas, including maternal care, behavioral health, and health equity. GetWell Navigate resides at the intersection of clinical and non-clinical. It enables better quality care. It improves outcomes. It delivers on the promise of personalized care for all.
How it works
AI-driven native text outreach
No app to download. Real people and AI-driven text messaging maximize engagement and extend reach to standardize trusted relationships.
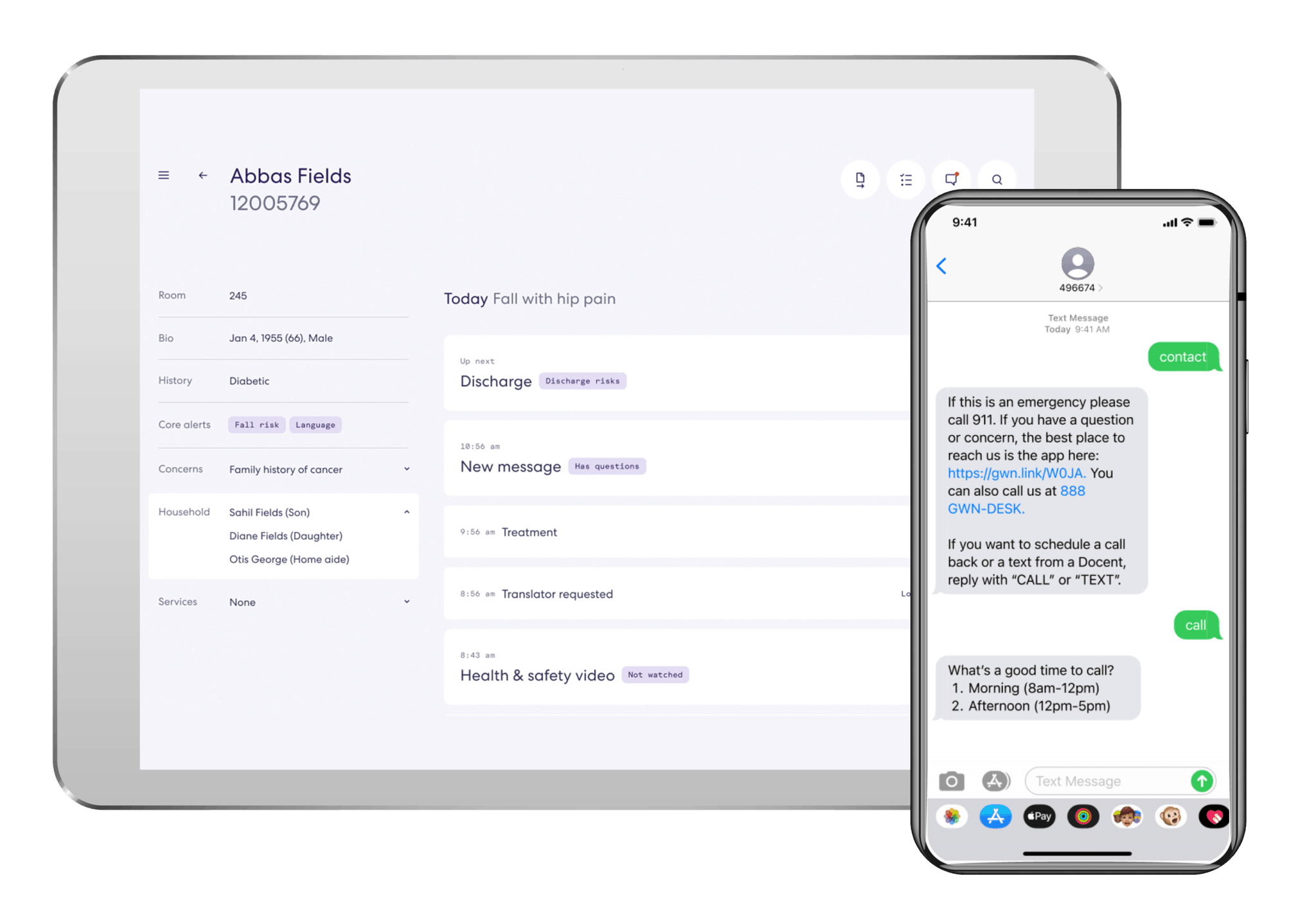
360-degree patient profile
Capture new behavioral, social, personal, and clinical data with integrations to track every interaction with the patient over time across the system.
Automate care pathways
Monitors patients in real-time and pinpoint opportunities, launches care pathways, and surface personalized recommendations and community resources to patients and next best actions to teams.
Ability for human intervention (yours or ours)
Intelligent workflows with AI texting scale patient-facing teams and enable empathetic interventions between people when it matters most. Tech-enable your teams or work with our community-based staffing solutions.
Why leading organizations choose to partner with us
Increase patient retention
GetWell Navigate reaches out and engages dormant patients or ACO patients and guides them to easily schedule in-network routine care before costs and complications escalate.
- 34% percent of patients scheduled with in-network PCP visit post-ED discharge
- 21% percent of dormant patients scheduled for in-network PCP visit
- $13M in lifetime value created
- 11 x ROI
Digitally enable population health
GetWell Navigate’s AI-driven texting and care coordination tools allow health systems and health plans to extend the reach of their services across the population to identify and support vulnerable and rising risk patients.
- 1% opt-out rate
- 10% increase in PCP appointments
- 17% increase in portal adoption
- 37% reduction in preterm births
- Health equity improvements across programs
Leveraging the power of artificial intelligence
No communication is as widely used as text messaging — 97% of people own a cell phone. Available to non-smartphone device users with no app download or Wi-Fi needed, it’s simple and convenient for all ages. It’s an ideal solution for every health plan and health system.
Using conversational artificial intelligence (AI), GetWell Navigate can manage single-person communications at scale, in a cost-effective manner. AI-driven SMS patient texting enables organizations to interpret, react, and learn from even the most complex interactions. Get Well Navigate’s AI text support offloads work, automating engagements that still personalize care. These interactions create scale, while facilitating engaging, proactive communication with patients.
Combine digital with human touchpoints
Even the best AI is improved when complemented by human touch. For unique patient questions or one-off requests, GetWell Navigate triggers and escalations allows for timely human intervention across the right channel.
These centralized, human and digital touch points throughout a patient’s healthcare journey provide a more empathetic and personalized care experience that takes health inequities into account. This mix of technology and human empathy is also proven to drive better outcomes, increase engagement, and build trust and relationships with today’s healthcare consumers.
By adding a conversational, more personalized, and empathetic element, GetWell Navigate can help ease the burden for staff caring for medically complicated patients who may be navigating transitional care programs and facing unique social determinants of health.
This leads to:
- Better quality care
- Reduced costs
- Closed critical gaps in care
- Increased personalization
- Established trust between patients and healthcare organizations
- Improved health equities for vulnerable populations
- Scaled effective care teams
By relying on proven technology, providers and staff are freed to focus their time and efforts on the human element – at scale.
Accelerate care
GetWell Navigate seamlessly guides people to timely support and services, without traditional barriers.
Gain efficiency
Boost care team efficiency, extend the reach of the care team, and deliver targeted business results with a care coordination workflow platform that allows you to reach more patients through automated text outreach. Through and 2-way texting with patients, GetWell Navigate enables escalations to the care team when human intervention is needed.
Achieve ROI
Drive ROI by delivering elevated care that engages patients, providers and health plans––resulting in cost savings and valuable growth.
Improve retention
Provide today’s healthcare consumers the experience they expect. We give you a modern way to build loyalty and brand awareness, retain known patients and bring back those with gaps in care, and attract new consumers.
100%
increase in resource utilization
78
global net promoter score
2x
downstream retention
4x
return on investment
Close care gaps and engage patients
Improving the overall health and wellness of a population or community is dependent upon the ability of individuals to receive care. But many patients simply don’t know what care they need or find it too difficult to figure out where to get it.
Re-engage patients in their care
People often skip appointments with their primary care providers, such as annual wellness visits. The COVID-19 pandemic has made this an even more critical issue. With Get Well Navigate, organizations can drive new volumes by re-engaging patients who have gone inactive, encouraging utilization of healthy behaviors and guiding patients to seek needed care in-network.
Identify patients for specific outreach
Many people also fail to engage in regular health maintenance, such as annual health screenings. GetWell Navigate enables personalized outreach to patients who are in need of routine procedures, such as mammograms, prostate exams, colonoscopies, and other screenings that are vital to maintaining health and wellness.
Serve the underserved
Underserved populations tend to engage with routine care even less than other communities. GetWell Navigate can reach underserved populations by:
- Engaging patients who receive Medicaid, including patients who are Medicaid/Medicare dual eligible
- Encouraging and supporting access to COVID-19 vaccinations
- Addressing behavioral health needs
- Assess social determinants of health needs and connect patients to community resources
- Promoting community-based human support to help overcome historical trust and cultural barriers to care
Tech-enable your care team
Ensure your teams are engaging with patients at the right time through their preferred channels. Established best practices can be individualized, so your teams can deliver personalized engagement to patients at scale.
GetWell Navigate arms your care teams with technology needed to seamlessly interact with and engage patients.
Reach more patients
GetWell Navigate monitors patients in real-time and pinpoints opportunities, automatically launches care pathways, and surfaces personalized recommendations and community resources to patients and next best actions to teams.
Improve care coordination
Improve coordination of care and ensure patient relationships are meaningfully shared to team members. With care team escalations, inpatient resolution boards and access center hand-offs, your care team has the technology it needs to efficiently and efficiently reach patients.
Increase transparency
View the full timeline of interactions with a patient, as well as scheduled future interactions. A comprehensive catalog of communications included in the timelines results in seamless transitions and a frictionless patient journey.
Provide holistic patient profiles
Inspire empathy by providing your teams with a whole person view of each patient through custom profiles.
Address healthcare disparities and improve health equity
Many people face unacceptable barriers to care because of their race, ethnicity, immigration status or geographic location. In November of 2020, 14 of the nation’s largest health systems announced a commitment of $700 million toward community-based initiatives aimed at addressing the economic and environmental drivers behind a widening disparity in health outcomes.
Get Well works with your organization to eliminate these disparities and create a more equitable healthcare system for all.
Holistic and extended engagement
Eliminate silos by partnering with local healthcare providers, proactively engaging with patients and building local community partnerships. The combination of social services and alternative care models enables healthcare organizations to support the unique needs of people where disparities exist.
Culturally competent & local
GetWell Navigate’s virtual care guides are locally hired and reflect the demographics of the communities they serve. Teams undergo implicit bias training and work to advocate for and guide their communities to better health.
Tech-enabled
Tracking and understanding the non-clinical side of the patient experience is critical. Are your team with applications to personalize and scale services for your organization.
Ecosystem Integration and collaboration
GetWell Navigate seamlessly integrates with your internal teams, as well as community resources, so patients get connected to the right resources, at the right time.
Data and measurement
Capture patient-reported data across a wide spectrum of measures. Integrations with provider partners and aggregation of public health data allows for a robust view of the patient and community.
Social determinants of health
Social determinants of health are non-clinical factors that affect a person’s health, such as socioeconomic status, access to healthcare, education level, exposure to stigma, and experiences with racism.
Through automated web surveys and patient texting, GetWell Navigate helps you capture social needs directly from patients with higher frequency and quality.
Resource mapping and matching
Improve personalized referrals to resources and services offered by your health system, third parties, and community-based organizations. You can choose to pair the application with your existing SDOH software to boost engagement in local resources or manage resources directly through GetWell Navigate.
Close the loop with patients
Follow up with patients over time to ensure they receive the support they need and monitor evolving needs.
Reporting and insights
Optimize your organizational partnerships with patient-level and aggregate reporting. Paired with GetWell Navigate insights, you’ll benefit from real-time reporting and analytics.